
Patellofemoral Pain Syndrome
The Use Of Electromyographic Biofeedback For Training The Vastus Medialis Obliquus In Patients With Patellofemoral Pain.
Charles R.Felder,
PT, SCS, ATC
Maureen A. Leeson, B.App.Sc.(Phty)
Introduction
Patellofemoral pain is a common ailment affecting one in four of the general population(6). It is caused by a variety of factors including abnormal lower limb mechanics, Vastus Medialis Obliquus (VMO) insufficiency, tight lateral structures and tight anterior and posterior muscles. The condition often develops gradually and is characterized by a diffuse ache in the area of the anterior knee. Pain is a significant factor since it will inhibit muscular activity and alter lower limb function. Anterior knee pain is often diagnosed as chondromalacia patella(2). This diagnosis is only correct when a softened and fissured patellar under-surface is seen during diagnostic imaging or surgery(2). Often, no cartilaginous pathological findings are present in patients who otherwise complain of severe knee pain and functional disability, especially during prolonged sitting, stair climbing or sporting activities.
The VMO muscle is the dynamic medial stabilizer of the patella. Therefore it is important to understand the anatomy and function of the VMO when treating patients with patellofemoral dysfunction. The fibers of the VMO insert into the patella at an angle of 50-55 degrees from the vertical axis(10)(see figure 1). The VMO is active throughout the full range of extension of the knee and is the only dynamic medial stabilizer of the patella(4). Insufficiency of the VMO will contribute to lateral tracking of the patella(3). Training the VMO is important to prevent lateral tracking of the patella and eliminate patellofemoral dysfunction.
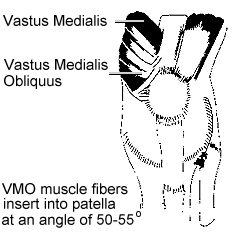
Figure 1. VMO insertion into patella
Electromyographic(EMG) studies of non-painful knees show that the ratio of VMO to Vastus Lateralis (VL) activity is 1:1 and that the VMO activity is tonic in nature(7). In knees with patellofemoral pain the VMO:VL ratio is less than 1:1(5,7) and the VMO activity becomes phasic in nature(8). This change in VMO activity may be the result of the asymmetric wasting of the Quadriceps muscle. Spencer et al(9) reported that it takes 20-30 ml of fluid to inhibit the VMO, whereas 50-60 ml of fluid is necessary to inhibit the VL activity. This asymmetry may result in lateral tracking of the patella, which is a common cause of patellofemoral pain.
MANAGEMENT OF PATELLOFEMORAL PAIN
The management of patellofemoral pain involves, first, a thorough analysis of the problem to identify the contributory factors; and second, correcting these problems. Lower limb mechanics are assessed and the alignment of the patella is evaluated. Patellar alignment is improved with tape and muscles are trained to optimize dynamic control. Taping the patella into correct alignment has been shown to increase EMG activity of the VMO, increase muscle torque and decrease pain (6). Change in the muscle activity of the knee improves patellar tracking and lower limb mechanics and significantly decreases pain.
EMG monitoring is utilized to assist with the assessment of muscle activity and to demonstrate any imbalance to the patient. The patient is then shown how to use EMG while training the VMO and VL. During training, the patient can use a portable EMG device to monitor the firing pattern of the muscles. Such a device can be used in a clinical setting as well as part of a home program. Training may also be specific to a particular part of the range of motion i.e. at 20-30 degrees of knee flexion, as the patella is engaging in the trochlear groove of the femur. As the VMO control improves, training progresses to include functional activities such as climbing stairs, squats, vocational and sporting activities, provided they are pain free ( see figure 2). In many instances, the problem is related to the timing of muscle contractions; when there is an imbalance of muscle activity, lateral tracking of the patella will result. This muscle imbalance can be demonstrated with EMG. Training may require subtle shifts in the timing of activity of the VMO:VL muscles. A portable EMG device provides the patient with instant feedback on the VMO activation (single channel EMG) or a comparison of VMO to VL activity (dual channel EMG). It then becomes easy for the patient to change the timing or the quantity of VMO activity (single channel) or VMO to VL activity (dual channel). The patient can progress to monitor his/her effort in functional or sporting activities. For example a ballet dancer can monitor the firing of the VMO in a pli�, a tennis player can ensure activation of the VMO while hitting through the ball and a basketball player can check the VMO while landing from a jump, etc.
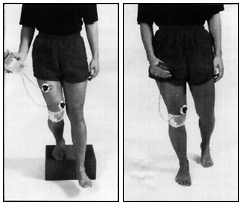
Figure 2. Training Exercises
Motivating patients to train the muscles is easier when they understand the underlying mechanism contributing to the problem. Training becomes an integral part of the patient's day to day living as well as sporting and recreational activities. Skill is enhanced and maintained with practice(1).
CASE HISTORY
A 35 year old male complained of right knee pain. He had a history of patellar subluxation and had undergone an arthroscopic medial menisectomy 8 years earlier. X-rays revealed early arthritic changes in the tibiofemoral joint. The patient's occupation as a photographer required him to walk, bend and squat frequently. His primary complaint was pain while at work and with recreational sports including tennis, downhill skiing and softball.
Objective examination showed an increased Q angle, pes planus, decreased VMO bulk and poor timing of the VMO to VL muscle activity. Step downs and partial squats reproduced the patient's pain. Patellar alignment tests revealed an inferior tilt, lateral tilt and external rotation. The lateral structures were tight, demonstrated by decreased patellar medial glide and medial tilt.
The patient's knee was taped to correct the patellar alignment. Patellar taping immediately resolved the patient's knee pain produced by partial squats and step downs. He was instructed in localized stretching for the lateral structures. The EMG sensors were applied to the VMO and VL and a training program was implemented to improve the VMO's timing and endurance. The EMG feedback helped the patient to monitor his VMO activity and change the timing of VMO to VL activity. It provided encouragement to activate an earlier, stronger, and longer VMO contraction. He trained at home, frequently, for short periods and eliminated his symptoms within six weeks. There was a total of three clinical visits. A one year follow-up call revealed continued absence of symptoms and the patient had returned to full functional activities without pain.
USING THE MYOTRAC EMG MONITOR
The MyoTrac single channel EMG monitor from Thought Technology helps the patient train the VMO by reinforcing the appropriate activity and monitoring fatigue. To accelerate the rate of learning, gain and threshold settings are adjusted to raise the level of difficulty. The visual and/or auditory feedback reward the patient for consistence in training and quality of effort.
Internal Settings
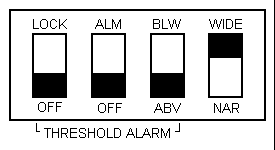
Figure 3. Internal Panel
- Lock in OFF position
- Alarm in OFF position
- Above/below switch set to ABV
- Bandwidth set to Wide (fig. 3)
External Settings
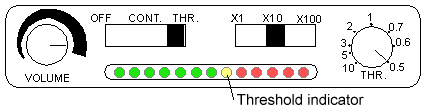
Figure 4. External Panel
- VOLUME: Turn clockwise to maximum if not using the earpiece. If using the earpiece, adjust the sound to a comfortable level
- OFF/CONT/THR: Set switch to THR
- Gain: Set switch to X10
- Threshold Dial: start with a 0.5 setting and turn counter clockwise to increase difficulty
- Connect the sensor to the appropriate jack
- Snap the self adhesive electrodes to the sensor
- Plug in the earpiece if desired (fig. 4)
Electrode Placement
- The patient sits in a chair with the foot on the floor and leg relaxed.
- The electrodes are placed over the VMO with the 2 active electrodes parallel to the orientation of the muscle fibers (see figure 5).
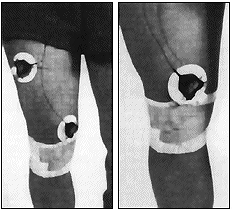
Figure 5. Electrode placement for single and dual channel EMG
TECHNIQUE FOR VMO TREATMENT
With the EMG monitor's gain at X10 and the threshold set to 0.5, if the first yellow light is on when the leg is relaxed, then the threshold dial should be turned counter clockwise (toward the higher numbers), until the green lights come on. If the first yellow light does not turn on with patient effort and the threshold dial is set to 0.5, then the unit should be adjusted to a more sensitive gain setting (i.e. X1). Once the green lights are on, the patient performs a Quadriceps contraction, ensuring that the VMO is recruited before or at the same time as the VL. The first yellow light indicate that the desired contraction is achieved (threshold). Ensure that the patient is achieving a quality contraction of the VMO with minimal activity of the VL. To achieve maximum benefit from the exercise, effort is required to activate the lights to the right of the threshold indicator and the sound. However quality of contraction, rather than quantity of contraction is of utmost importance. If the threshold dial is turned to 10 and the patient still finds it easy to perform a VMO contraction and activate the first yellow light, the scale is switched to X100 and the threshold returned to 0.5.
The patient progresses to using the MyoTrac to monitor the VMO function in all of his/her functional training. The patient also learns to identify VMO fatigue during treatment and is told to stop when fatigue occurs so that training does not continue in an inappropriate pattern. After a brief rest, training is resumed, ensuring that the VMO is recruited before or at the same time as the VL.
Simultaneous monitoring of the VMO and VL with a dual channel EMG allows for comparison of the timing and contraction and will assist the patient to train the timing component. The firing pattern can be monitored by two MyoTrac units used simultaneously; one to monitor the VMO and one to monitor the VL. Alternatively the dual channel MyoTrac 2 can be used to monitor both muscles.
USING MYOTRAC 2 FOR PF PAIN
The MyoTrac 2, also from Thought Technology, is a dual channel EMG monitor similar to the MyoTrac but with a numeric readout in addition to the visual (LED) feedback and audible tone. With the aid of the digital readout (displaying absolute micro-Volt levels), it becomes easy to demonstrate to the patient the initial asymmetry between the VMO and the VL activity. As well, this permits an easier visualization of the effect of training. The MyoTrac 2 also permits the recording of the patient's training sessions, thus allowing to demonstrate progress of training over time. The stored data may be downloaded to a printer for documentation purposes, or downloaded to an IBM compatible computer for further analyses.
Initial Setup
(Do this only once, settings are saved automatically for subsequent use)
- Press 'On/Off' and wait for the unit to be initialized
- Press 'Channel Settings', get the 'Filter' settings by pressing 'Enter' and confirm that both are set at 20-500 Hz. If not, press the 'UP' or 'DOWN' arrow keys to change the settings
- Press 'Esc'
- Press the 'DOWN' arrow once to access 'Channel Ranges' and press 'Enter'
- Make certain that the ranges are 0-250 micro Volts (uV); if not, change them by using the 'RIGHT' or 'LEFT' arrow to switch channels and the 'UP' or 'DOWN' arrow to change the range. Press 'Esc'
- Press 'Sound'
- Turn the speaker ON (if OFF) by pressing 'Enter'
- Press the 'UP' arrow once to get the 'Volume' setting. Press 'Enter' and use the 'UP' arrow key to set the volume to 9; change to channel 2 by pressing the 'RIGHT' or 'LEFT' arrow and do the same thing. Press 'Enter'
- Press the 'UP' arrow once more to get 'Above/Below' setting and 'Enter'
- Set to 'Above Thresh.' for both channels and press 'Enter'
- Press 'UP' again to get the 'Sound mode' settings and 'Enter'
- Select 'Thresh/prop.' for both channels and press 'Enter'
- Press 'Record'. Press the'UP' arrow twice to get 'Cont Chan Save'. Press 'Enter' Make sure that both channels are set to OFF.
- Press 'UP' once more to get 'Cont. Statistics'. Press 'Enter' and make sure that all three options, 'Avg', 'Min' and 'Peak' are set to 'Yes'.
Note: You can also use ratio feedback to monitor a VMO:VL greater than 1:1 by choosing the 'Ratio' display (see the MyoTrac 2 User's Manual).
TRAINING WITH MYOTRAC 2
- Place the electrodes over the VMO and VL muscles
- Plug in the earphones, if desired
- Press 'Display'
- Press the 'UP' arrow once to get 'Peak and Actual'. Press 'Enter'
- Set 'Auto/Manual' to manual (Man'l:use TimeMk) by pressing 'UP' once. Press 'Enter'
- The screen displays the immediate activity on the right and the peak activity on the left for both channels
- You can set the threshold levels by pressing 'Threshold' and using the 'UP' and 'DOWN' arrows to increase and decrease the values. Switch channels by pressing 'Enter'. It is a good idea to set the VMO level slightly higher, to reinforce greater activity in that muscle group. Return to the 'Peak and Actual' display screen by pressing 'Display', 'UP', 'Enter' and 'Enter' again.
- After each contraction of the VMO and VL, observe the peak values for each contraction/relaxation cycle. Then press 'Time Mark' to reset the peak to the current value.
- If you wish to record this data, press 'Record'. The MyoTrac 2 displays the 'Time segment Recording ON' message. Each time you press 'Time Mark' the max, min and average values are saved.
CONCLUSION
Clinical evidence shows that the VM and VL muscles can be trained specifically to align the patella(6). Ongoing and regular training will produce effects that are beneficial and long term, and the patient can remain free of pain even while participating in activities which are demanding on the patellofemoral joint. Using a single or dual channel EMG device to monitor the VMO and evaluate the patient's progress is the key to success.
References
- Englehorn R :Agonist & Antagonist muscle EMG activity pattern changes with skill acquisition. Research Quarterly for Exercise and Sports, 54(4): 315-323 1983.
- Fulkerson, JP, & Hungerford DS: Disorders of the Patellofemoral joint, 2nd edition. Williams and Wilkins Co, 1990.
- LeVeau B & Rodgers C: Selective training of the vastus medialis muscle using EMG biofeedback. Physiotherapy 60 (11): 1410-1415, 1980.
- Lieb R & Perry J: Quadriceps function. JBJS 50A (8): 1535-1548, 1968.
- Mariani P. & Canuso: An electromyographic investigation of subluxation of the patella. JBJS 61B: 169-171, 1979.
- McConnell J.S.: the management of chondromalacia patellae: A long term solution. Australian J Physiotherapy 32 (4): 215-223, 1986.
- Reynolds L, Levin T, Medeiron J, Adler N, & Hallum A: EMG activity of the vastus medialis oblique and vastus lateralis and their role in patellar alignment. American J. of Physical Medicine, 62 (2): 61-71, 1983.
- Richardson C: The role of the knee musculature in high speed oscillating movements of the knee, MTAA 4th Biennial Conference Proceedings, Brisbane, 59-70, 1985.
- Spencer J, Hayes K, & Alexander I: Knee joint effusion and quadriceps reflex inhibition in man. Arch Phys Med, 65: 171-177, 1984.
- Terry G. The anatomy of the extensor mechanism. Clinics in Sports medicine 8 (2): 163-177, 1989.
Copyright, 1997 The Biofeedback Federation of Europe