|
|
Phantom
Limb Pain
The Use of EIectromyographic
and Temperature Biofeedback for Treatment of Cramping and
Burning Phantom Limb Pain
Richard A
Sherman, Ph.D
LTC, Medical Service, US Army Chief,
Clinical Biometrics Service
Dept. of Clinical Investigation
Fitzsimons Army Medical Center Aurora , CO.
Introduction
Virtually everybody who has had an amputation reports
feeling sensations which appear to emanate from the
amputated portion of the limb. Most of the time, these
"phantom" sensations are painless and of
sufficiently low intensity to be no more than a mild
distraction(9). The sensations are usually similar to
those which would be felt in an intact limb, including
warmth, itching, sense of position, and mild squeezing.
Awareness of details of the limb's shape and perceived
ability to move it tend to fade with time. However,
almost all amputees report continuing to feel at least
some phantom sensations throughout the remainder of their
lives. When phantom sensations become intense enough for
the amputee to define them as painful, they are called
"phantom pains". The neural mechanisms which
permit perception of phantom limbs are well
recognized(3,4). Sensations reaching the brain are
identified for location on the skin by the homunculus, in
the sensory cortex, which contains a representation of
the entire body surface. Thus, a pinch of the left index
finger tip stimulates a location on the homunculus
representing the left index finger tip.
If the finger was amputated and a signal was started
by pressure, etc., anywhere along the remaining nerve
paths between the finger stump and homunculus, the
resulting sensation would seem to emanate from the finger
tip because the paths do not change much after amputation
and the brain has no way to know that the finger tip is
not present.
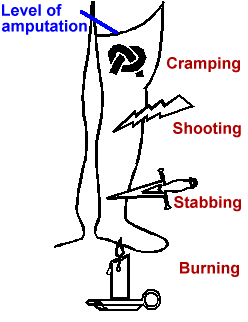
Figure 1. Common descriptions of phantom pain
Phantom limb pain occurs among between 50 and 80
percent of amputees(9,10). The most common descriptions
of phantom pain are variants of cramping,
burning/tingling, and shocking/shooting/stabbing (Fig.
1). Each amputee tends to report the same one or two
descriptions of phantom pain whose locations within the
phantom remain consistent over time. A large minority
have episodes severe enough to interfere with work, sleep
and desired social activities which occur frequently
enough to require treatment.
Phantom pain can occur anytime, from just after an
amputation to years later. Its occurrence is not related
to psychological factors(12), age, sex, location of the
amputation, or reason for the amputation (e.g. trauma vs.
disease). Different individuals report their phantom
pains to be affected by different environmental variables
such as changes in humidity and temperature(2,10). As is
true with all chronic pain syndromes, stress and fatigue
can magnify the sensations but there is absolutely no
evidence that any psychological factors cause phantom
pain(1,12). Pain from pinched nerves in the back and
other sources is referred to the phantom limb as it would
be to the original limb.
Recent surface electromyographic studies(8,11) have
demonstrated that the major muscles in the residual limb
tense up several seconds before the cramping phantom limb
pain begins and that these muscles remain tense for much
of the duration of the episode. The pattern of tensing is
usually shown by an abrupt increase in magnitude of
surface electromyogram to about twenty times baseline
values. Other studies(6) have demonstrated that burning
phantom limb pain is closely associated with reduced
blood flow in the residual limb. There is currently no
evidence associating shooting/shocking descriptions of
phantom pain with specific physiological mechanisms.
However, very similar sensations are provoked during
ectopic stimulation of nerves from a neuroma.
In the past, the success rate for treatment of phantom
pain has been dismal, with only about one percent of
treated amputees reporting effective relief lasting for
at least a year(9,10). At least forty-three ineffective
treatments were in common use until recently(10). They
range in invasiveness from lobotomies and major spinal
surgery, through surgical revision of the residual limb,
psychotherapy, and psychoactive drugs, to transcutaneous
electrical stimulation and similar techniques. The only
treatments consistently able to ameliorate phantom pain
were sympathetic locks and sympathectomies which were
useful for burning phantom pain for up to a year.
Current treatments are based on the mechanisms
discussed above and have been proven to be more
effective(5,7). Cramping phantom pain responds well to
treatments which result in preventing the residual limb
from tensing up abnormally, while burning phantom pain
responds well to treatments which increase blood flow,
both in and out of the residual limb. No treatments have
been identified as being consistently effective for
shocking/shooting descriptions of phantom pain. The
diagnostic decision making process for choosing the
treatments most likely to be effective for different
descriptions of phantom pain has been detailed
elsewhere(3).
Biofeedback
Treatment
For patients who describe burning/tingling phantom
limb pain and have an essentially normal reactive
vascular system, a trial of temperature biofeedback may
provide relief. We start these patients out with surface
electromyographic biofeedback because we find that it is
easier to learn and gives trainees the confidence they
need when learning to control their limb temperature. If
the patient describes cramping/squeezing phantom limb
pain, and is able to learn control of the voluntary
muscles, a trial of surface electromyographic biofeedback
is appropriate. Amputees who give mixed descriptions of
phantom pain which include shocking/shooting sensations
may have success learning to control other descriptions
of phantom pain but the shocking/shooting sensations are
likely to remain unchanged. Amputees reporting combined
burning and cramping pain are given treatments aimed at
controlling both underlying mechanisms.
The specific aim of the treatment is to teach amputees
with burning/tingling phantom pain to habitually and
unconsciously keep their residual limbs as warm as the
intact limb. For amputees with cramping pain, the aim is
to teach them to prevent the onset of the types of
increases in muscle tension in the residual limb which
lead to pain. These aims are approached through several
overlapping stages:
- First, subjects are shown the relationship
between the residual limb's temperature or
muscular activity and the onset and intensity of
phantom pain, so they are absolutely convinced of
the relationship.
- Next, they are given muscle tension and
temperature awareness training very similar to
Jacobson's system. They are given tape recorded
exercises to play at home at least twice per day.
The aim of this phase is to begin increasing
their awareness of changes in limb temperature
and tension patterns as well as to begin helping
them learn to control these parameters.
- After several weeks, the tapes are used only once
per day and the patients begin doing the exercise
on their own at least once at home and once while
out in their normal work environment. This is
intended to begin generalizing their awareness of
changes in the parameters to their normal
environment.
- The week after, subjects begin home training,
they participate in weekly or biweekly
biofeedback sessions conducted in the clinic. The
sessions follow the guidelines detailed in the
Association for Applied Psychophysiology and
Biofeedback's application standards manual(14).
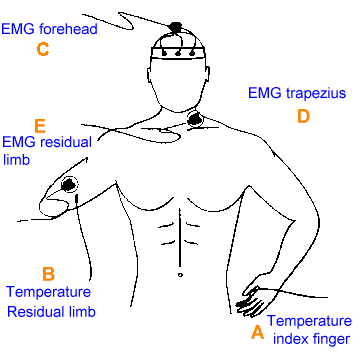
Figure 2. Placement of EMG and temperature
sensors
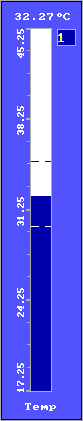
Figure 3.
Bar graph |
- Subjects being taught temperature
biofeedback begin by having the
dominant index finger
instrumented with a single
temperature sensor (fig. 2A). If
neither hand is present, the toes
are used. Skin temperature is fed
back to the patient from both a
line graph or bar graph display
(fig 3, 4) and an auditory signal
(illustrations are from Thought
Technology's ProComp+/DOS
biofeedback system).
- They continue to receive training
for this area until they
demonstrate the ability to
consistently and reliably raise
their finger temperature. We do
not normally either have patients
work to a preset goal or require
the ability to quickly raise,
lower, and then raise finger
temperature, because achievement
of these goals does not seem to
relate to symptom control.
Instead, we tailor each treatment
to the individual's ability to
raise temperature.
|

Figure 4. Line graph
|
|
After control is demonstrated in the finger, the
sensor is mounted on the warmest portion of the
residual limb (figure 2B) and ability to control
temperature of that area is trained. This is a
slow process which can take eight sessions or
more. The sensor should not be placed near the
end of the residual limb as the vascular bed, in
that area, is highly abnormal and most subjects
have not learned to control limb temperature when
the sensor is placed there.
Subjects who are being taught to recognize and
control muscle tension receive a similar program.
Their foreheads are insturmented with surface
electrodes (figure 2C) and signals are fed back
through a light bar or auditory display (figure
5.) Picture of MyoTrac 2 Dual channel EMG
system provided by Thought Technology Ltd.)

Figure 5. Light bar feedback display
Instruct the patient to lower the tone and light
bar readings. When they can demonstrate the
ability to reliably relax the facial muscles, the
sensors are moved to the right or left trapezius
sites where similar training is performed (figure
2D).
After control is demonstrated, place the EMG
electrode over one of the major muscles of the
residual limb (figure 2E) and teach the subject
to recognize tension patterns by controlling
muscle tension in the limb. This process can take
twelve sessions or more.
Awareness of the residual limb's temperature
and/or patterns of muscle tension in the
patient's environment is emphasized throughout
the training process so that control is
eventually achieved while the subject is in the
normal environment without the subject having to
concentrate on continuously maintaining control.Conclusion
Biofeedback can be an effective treatment for
cramping and burning phantom limb pain when used
with appropriate patients in conjunction with
home based temperature and muscle tension
recognition and control training. This modality
should be attempted before using medication or
other invasive therapies as it is at least
equally effective and relieves patients of the
need for continuing use of drugs which usually
have deleterious side effects.
REFERENCES
- Arena. J., R. Sherman, G. Bruno and J.
Smith: The relationships between
situational stress and phantom limb pain:
Cross-lagged correlational data from six
month pain logs. Psychosomatic Research,
34: 71-77 (1990).
- Arena, J., R. Sherman and G. Bruno: The
relationship between humidity level,
temperature and phantom limb pain:
Preliminary Analysis. Biofeedback and
Self-Regulation, 14: 128 (1989).
- Sherman, R.: Phantom limb and stump pain.
In Neurologic Clinics of North America. (Portenoy. R. Ed.) Philadelphia,
W.B.
Saunders Co. (1989).
- Sherman, R., J. Arena and J. Ernst: The
mystery of phantom pain: Growing evidence
for physiological mechanisms. Biofeedback
and Self-Regulation, 14(4): 267-280
(1990).
- Sherman, R., Arena, J., Griffin, V.,
Bruno, G., Cocilovo A.: Biofeedback for
the treatment of phantom limb pain: An
update. Biofeedback. 7(3): 7-8 (1991).
- Sherman, R. and G. Bruno: Concurrent
variation of burning phantom limb and
stump pain with near surface blood flow
in the stump. Orthopedics, 10: 1395-1402
(1987).
- Sherman, R., N. Gall and J.
Gormly:
Treatment of phantom limb pain with
muscular relaxation training to disrupt
the pain/tension cycle. Pain 6: 47-55
(1979).
- Sherman, R., V. Griffin, C. Evans and A.
Grana: Temporal relationships between
changes in phantom limb pain intensity
and changes in surface electromyogram of
the residual limb. International Journal
of Psychophysiology, In Press, 1992.
- Sherman, R. and C. Sherman: Prevalence
and characteristics of chronic phantom
limb pain among American veterans. Am. J.
Phys. Med. 62: 227-238 (1983).
- Sherman, R. and C. Sherman: A comparison
of phantom sensations among amputees
whose amputations were of civilian and
military origins. Pain 21: 91-97 (l985).
- Sherman, R. and C. Sherman: Physiological
parameters that change when pain changes:
Approaches to unraveling the
"cause-or-reaction" quandary.
Bulletin of the American Pain Society.
1(4): 11-15 (1991).
- Sherman, R., C. Sherman and G. Bruno:
Psychological factors influencing chronic
phantom limb pain: An analysis of the
literature. Pain 28: 285-295 (1987).
- Sherman, R., C. Sherman and L. Parker:
Chronic phantom and stump pain among
American veterans: Results of a survey.
Pain 18: 83-95 (1984).
- Biofeedback Applications Manual,
AAPB,
1991.
Acknowledgments and Disclaimer
Figure 1 was originally finalized by Karen
Wyatt, Medical Illustrator at Fitzsimons Army
Medical Center, from a draft provided by the
author. The manuscript was reviewed by Vernice
Griffin and Cecile Evans of the Psychophysiology
Laboratory at Fitzsimons Army Medical Center. The
work reported here was entirety supported by the U.S, Army and the Department of Veterans Affairs.
However, the opinions and assertions contained in
this manuscript are the private views of the
author and are not to be construed as official or
as reflecting the views of the United States
Departments of Veterans Affairs, Army or Defense.
Copyright, 1997
The
Biofeedback Foundation of Europe
|